Your visit for routine eye care allows your eye doctor to evaluate your visual needs. The doctor can determine if there is a need to prescribe or change your prescription for vision correction. It also allows him/her to evaluate your eye health, to rule out the most common eye diseases and to determine if there is a need for further evaluation and procedures.
Vision insurance is usually a separate insurance covered by your employer or insurance company that covers routine eye care and may or may not include payments towards eyeglasses or contact lenses. It cannot be used to treat medical problems. Medical eye care involves visits and procedures your doctor performs to diagnose and to treat eye disease such as glaucoma, dry eye, conjunctivitis and cataracts. It may or may not include determination of your eyeglass prescription.
Many of the examinations and tests performed at SUNY College of Optometry evaluate your eyes for possible disease. Once a disease is found, examinations and tests allow us to manage your eyes appropriately. There is however, one test called a refraction that is typically not covered by insurance that needs to be performed at least once a year. It is not an optional test, but essential to fully evaluate your eyes appropriately. Federal guidelines state that the office visit and the refraction are to be reported as two separate charges when submitting your services to Medicare and other insurances. Most medical insurance carriers do not cover charges for the refraction and there is a separate charge for this service. The payment for the refraction must be made at the time of service along with your copay and any deductible amounts for the covered charges for your visit.
Recommended Examination Frequency for Pediatric Patients
| PATIENT AGE | EXAMINATION INTERVAL | |
|---|---|---|
| Asymptomatic/Risk Free | At Risk | |
| Birth to 24 Months | At 6 months of age | By 6 months of age or as recommended |
| 2 to 5 years | At 3 years of age | At 3 years of age or as recommended |
| 6 to 18 years | Before first grade and every two years thereafter | Annually or as recommended |
Children considered to be at risk for the development of eye and vision problems may need additional testing or more frequent re-evaluation. Factors placing an infant, toddler, or child at significant risk for visual impairment include:
Recommended Examination Frequency for Adult Patients
| PATIENT AGE | EXAMINATION INTERVAL | |
|---|---|---|
| Asymptomatic/Risk Free | At Risk | |
| 18 to 60 years | Every two years | Every one to two years or as recommended |
| 61 and older | Annually | Annually or as recommended |
Patients at risk include those:
You can pay your bill online either through your patient portal account. For billing questions please call 866-905-4477 Monday through Friday 9:00am-5:00pm.
In most cases, we can help establish a payment plan depending on your balances due. Partial payments made toward your balance will not stop collection activity unless you have made payment arrangements with us. Please contact Patient Financial Services to discuss payment options at Tel: 866-905-4477
We accept most Medicaid Medicare and most major medical and vision plans.
For a listing of our participating plans, please see link.
If you are uninsured or underinsured, you may qualify for a fee reduction based on specific financial eligibility. To apply for financial assistance, you will be asked to provide information, which includes financial income. We utilize the federal poverty levels as guide for fee reduction determinations. The federal poverty levels are listed below:
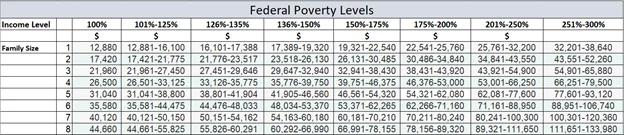
Please call 866-905-4477or email pfsfinapp@sunyopt.edu for information.
Vision care plans typically only cover routine vision examinations along with eyeglasses and contact lenses. Your visit for routine eye care allows your eye doctor to evaluate your visual needs. The doctor can determine if there is a need to prescribe or change your prescription for vision correction. It also allows him/her to evaluate your eye health, to rule out the most common eye diseases and to determine if there is a need for further visits. Vision plans do not cover diagnosis, management or treatment of eye diseases.
Today it is relatively common to have a vision benefit plan in addition to your medical insurance. This can lead to confusion about whether your medical or vision insurance should be billed. Once the doctor concludes your examination and determines the billing code and depending on your insurance benefits your medical or vision plan could be billed. Vision insurance is usually a separate insurance in addition to your medical insurance that covers routine eye care which includes a refraction. Your vision plan may or may not include payments towards eyeglasses or contact lenses. Vision benefits cannot be used to treat medical problems. If you are unsure of your benefits, please contact your insurance directly.
Medical insurance is used to diagnose and treat diseases. Your medical insurance should be used if you have any eye problems or diseases. Medical eye care covers visits and procedures your doctor performs to diagnose and to treat eye disease, such as glaucoma, dry eye, conjunctivitis and cataracts. It may or may not include determination of your eyeglass prescription.
You should use your vision benefit plan when you are not experiencing any ocular problems and only want a wellness exam or when you want to check if you need new glasses or contact lenses. Be sure to let us know the purpose of your visit when you schedule your appointment to lessen the chance of confusion as to whether the vision plan or the medical plan is the appropriate billing choice for the visit. If you have both types of insurance plans it may be necessary for us to bill some services to one plan and one to the other. We will bill your insurance plan for services if we are a participating provider for that plan. We will try to obtain advanced authorization of your insurance benefits so we can tell you what is covered. If some fees are not paid by your plan, we will bill you for any unpaid deductibles, co-pays or non-covered services as allowed by your insurance contract.